The Role of Herbs in Holistic Healing
Have you ever considered herbal remedies for Perimenopause symptoms?
In my podcast episode #19, I interview Chris Lamont, a registered herbalist and member of the Ontario herbalist Association. He is a manufacturer of herbal remedies and member of the OHA since 2015. In our conversation we talk about how midlife women can alleviate and even avoid perimenopause symptoms with self-care and some incredible herbal remedies.
Chris Lamont started his professional life as a musician. He is a rock star turned herbalist. He has spent a lot of time outdoors and is an ardent nature lover. He comes from a medical family that has instilled in him a love for healing. Chris leads workshops, works in the clinic, is the caretaker of a herb farm where he uses the grown herbs to make medicines and is a herbal remedy educator.
What is the biggest challenge for women going through midlife transition?
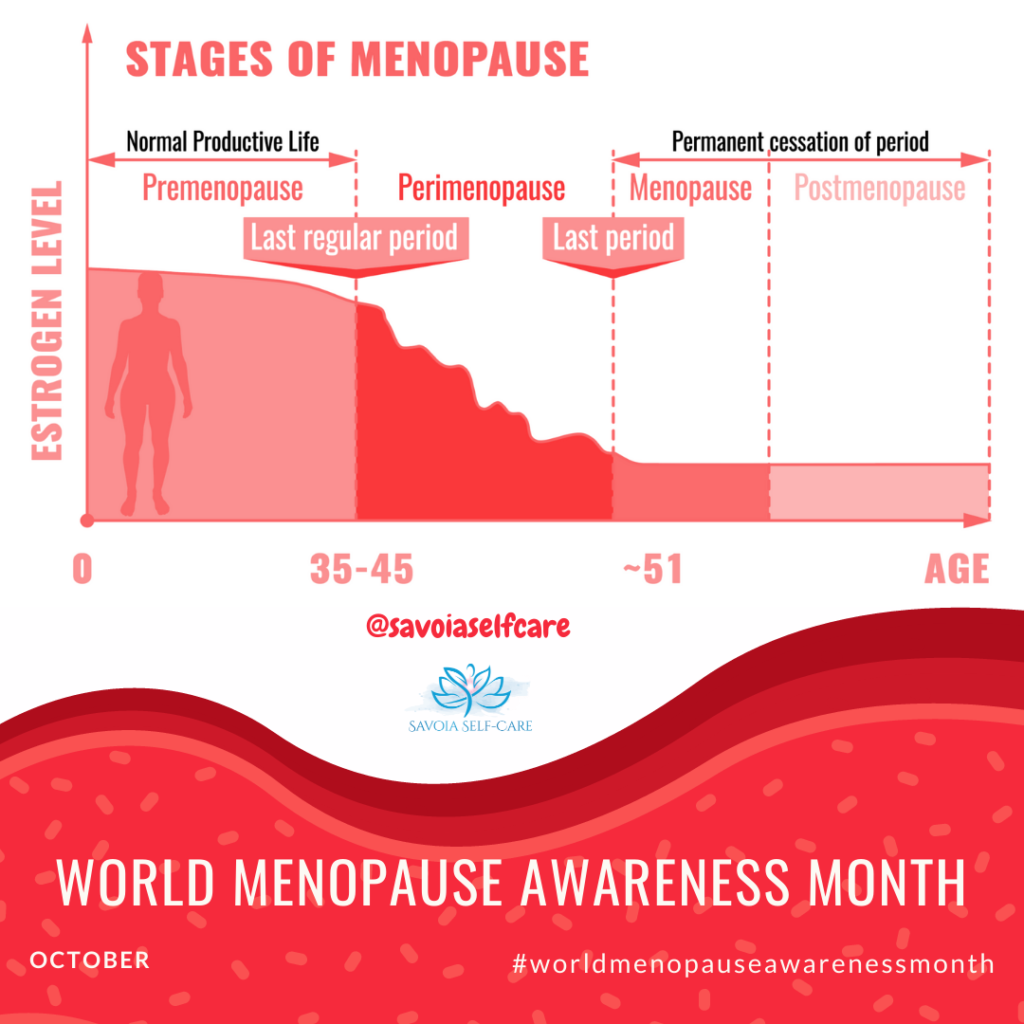
According to Chris Lamont what makes midlife transition difficult are the numerous symptoms and the uncertainty of what to expect. Because the probable symptoms are so vast such as weight gain, sleep issues, and mood changes, mental fog, low energy, hot flashes, and many, many more it is difficult to prepare for what is coming. Most women are also unable to accept their midlife transition on an emotional level. They feel a loss of womanhood associated with the end of their reproductive potential and a shift in sexual function. Chris says that the emotional component is more devastating and it is important for woman to understand that this is a natural process that all women go through. Menopause is not a loss of anything. It is a shift. He explains how Perimenopause usually starts in a woman’s mid 40’s and can last for 2-10 years. When a woman has not got her period for 12 consecutive months the phase is termed as Menopause and it is followed by the post Menopause period. Listen to my Perimenopuase 101 episode here.
Stereotypically, in North America Perimeopause is seen as a negative transition or a steep point in life. In other parts of the world as like an Asia, especially in Traditional Chinese Medicine, it’s actually called a Second Spring or a rebirth of a woman and I really believe it’s actually a better phase of life because you’re more certain of yourself, have seen more of life and you’re more mature. In my opinion this can even be looked at as a favourable stage in life. Interestingly a lot of Asian women do not have any of the symptoms that North American women do!
According to the Merriam Webster dictionary the term ‘climacteric’ means ‘critical point’ According to Chris, it is a term traditionally used to describe menopause as menopause is seen as the climax of the reproductive phase of life. This is a terrible way to look at menopause as it feeds the idea of loss. In fact women must be encouraged to approach this whole new phase of life by open discussions about the transition and just by feeling better about themselves. In Chris’s opinion prevention of the symptoms associated with perimenopause is an important part. Women should be aware on how to fortify their body so that if the symptoms show up they are a lot easier to handle. And how I always like to say Prevention is KEY.
What are the top symptoms during Perimenopause?
Chris points out that with any kind of holistic healing modality it is essential to identify the root cause of any situation. A remedial formula should be custom made to fit the exact needs of the person. Chris also advises to avoid using Dr. Google for self-diagnosis and treatment and opt for professional opinion to ensure the proper way of doing things.

- Weight Gain
This symptom is clearly visible to everyone in the outside world and affects the opinion we formulate about ourselves. Chris reinstates the fact that during Perimenopause there is loss of muscle mass and increase in body fat. The ovaries stop producing estrogen and other parts of the body such as the adrenal glands make estrogen, progesterone and fat cells. Premenopausal women need to be in good shape but not necessarily fat free. Getting into shape is one of the things that can be done as a preventative measure ahead of time, with the understanding that we don’t want to be super fit. Menopause correlates with an increase in insulin resistance. Glucose is now also stored as fat. There’s a natural push towards an increase in body fat. According to Chris we can prevent that by working hard to normalise blood sugar, and use the right herbs. He advises Perimenopausal women to watch their diet and make sure they are not predisposed to insulin resistance ahead of time. To address symptoms of weight gain we can use herbs that can help to manage blood sugar called hypoglycaemic herbs. These include foods like cinnamon, blueberry, fenugreek and garlic that can be used to help to normalise blood sugar and set us up for success ahead of time.
Why is most fat stored near the belly? Why the muffin top?
During Perimenopause the ovaries begin to slow down production of sex hormones creating low levels of estrogen in the body. This promotes visceral fat storage in the belly. Visceral fat is linked to the fat around our digestive organs and colon. This may cause health problems like diabetes and heart disease. Chris says that another factor is stress. There’s a higher ratio of cortisol receptors in the viscera, than the rest of the body. When pumping out cortisol, in our fight or flight state which is the body’s stress response, those receptors are more active. White fat is deposited more in the viscera than elsewhere. Thus, managing stress is extremely vital for Perimenopausal women.
In the podcast Chris explains that there are two hormones related to hunger. Ghrelin which is significantly higher among Perimenopausal women and leptin is the hormone that shuts down the hunger response. Leptin gives us the signal that we are satisfied and full. In the later stages of Perimenopause when we have low levels of estrogen it impairs the function of leptin. Our body does not get the normal signals of be satisfied or full. But there are herbal remedies that combat estrogen and progesterone hormonal imbalances and soften the estrogen deficit that can be tapped into during the Perimenopause transition.
2. Insomnia
Insomnia is the second most common symptoms amongst perimenopause women. Difficulty in sleeping could also be a secondary effect due to other symptoms like night sweats or hot flashes. Studies have shown that progesterone has a beneficial affect on sleep. During perimenopause the levels of progesterone decreases and our body produces less melatonin that leads to insomnia. There are different types of insomnia.
- Sleep Onset Insomnia – Difficulty falling asleep at the beginning of the night. This is stress or anxiety related or due to an overactive mind worrying about a to do list for the next day. This can be overcome with what Chris calls ‘sleep hygiene’. Develop a bedtime routine, limit screen time before bed, do not eat too late at night and ensure the room temperature is comfortable. If you think your mental activity is too high keep a notebook and pen beside your bed and unload your thoughts such as mistakes made the day before, things you are afraid you’ll forget or to do list for the next day onto paper to relax the mind. Along with these non-herbal ways there are herbal remedies that Chris Lamont advises with sleep onset are the sedative hypnotic herbs that relax the body or stronger herbs that make you feel drowsy.
- Sleep Maintenance Insomnia – Waking up consistently at 2, 3 or 4’o clock in the morning. This can be due to liver trouble or blood sugar problems. There are herbal remedies available for this as well.
- Waking up earlier than desired – This could be due to issues in cortisol production.
It is important to identify what type of insomnia we are dealing with and what is the root cause and provide an appropriate protocol.
3. Hot Flashes and Night Sweats
In a 2003 placebo-controlled research study 55 postmenopausal women were given Dong Quai and camomile instead of HRT (hormone replacement therapy) showed that they had 80{1e16acf445973e61fdbd53de1c132af7e84fd195cf15d57956db2b0426c8fa60} reduction in hot flashes after one month. This amazing result is not surprising as Dong Quai or Angelica Sinensis also called Chinese Angelica, is a fantastic hormone modulator and phytoestrogenic herb. Hot flashes and night sweats are symptoms that respond very well and quickly to herbal therapy.
Why do we get hot flashes and night sweats?
75{1e16acf445973e61fdbd53de1c132af7e84fd195cf15d57956db2b0426c8fa60} of women experience hot flashes and night sweats due to the interplay of the endocrine system. In Perimenopause the hypothalamus gets the message that estrogen levels are too low or fluctuating. The hypothalamus sends the message to the pituitary gland which releases a follicle-stimulating hormone. This stimulates the follicle in the ovary to produce more estrogen. When repeatedly the hypothalamus does not get the desired result, it floods the body with adrenalin. This causes body temperature reset causing a wave of heat. The blood vessels also become sensitive to temperature signals during Perimenopause. They dilate and bring heat to the surface more easily. This is what flushing is. Sweating is a method of releasing heat from the body. All of this is initiated in the brain as an attempt to correct the lack of estrogen. The thyroid gland oversees metabolism and one of the products of metabolism is the creation of heat. As a remedial measure Chris advises that apart from the basic hormone modulation and phytoestrogenic herbs, we can take herbs called adaptogens. They help the body deal with stress and take work off the adrenals. We can also consume nervous system herbs like Motherwort, Oats and Linden Flower. Sage is a drying herb that can reduce sweating. Chris advises that the easiest way to mitigate these symptoms is to temporarily avoid common triggers for night sweats and hot flashes during Perimenopause like caffeine, smoking, eating spicy foods, alcohol, tight clothing and dealing with stress and anxiety
4. Mood Symptoms.
These include mood shifts, mood swings, depression, anxiety, irritability, that not only affect yourself, but also affect your relationships and work. In the podcast Chris talks about how these symptoms are not in isolation but instead tend to shift between each other. Certain neurotransmitters like serotonin may cause these changes. Mood swings can be hormonal or a secondary result of other issues like insomnia. The less good quality sleep you get, the more grumpy or depressed or anxious you may feel.
Moods are intimately tied to our work, friend, family and romantic relationships. When our sexual function is impaired, it affects our mood in a huge way. Research has found that women who have severe PMS symptoms in their younger years, tend to have more severe mood swings during perimenopause. The herbal remedy depends on what is the predominant mood issue. For example, if depression is the main mood issue, maybe there is anxiety and we can use antidepressant herbs, stimulating adaptogens, which can help to elevate the mood.
The gut microbiome is responsible for our nervous system function and our mood. Our friendly gut bacteria produce majority of different neurotransmitters, serotonin, and dopamine. If our gut is not functioning properly and microbiome is compromised by use of antibiotics, stress, leaky gut syndrome, and inflammation, then we do not get enough neurotransmitters in the amounts that we need. We can do this ahead of time and get the gut in shape, optimise digestion, and that can go a long way in affecting mood. The gut produces 70-80{1e16acf445973e61fdbd53de1c132af7e84fd195cf15d57956db2b0426c8fa60} of serotonin which is the feel good hormone. Read more about the gut-brain connection in my earlier post here.
“It’s not your fault. At the end of the day, hormones rule the world”
The hypothalamus-pituitary-adrenal (HPA) axis is part of the endocrine system. If the ovaries or the adrenals are out of whack it will affect the rest of the system because they all work together in harmony. The hypothalamus, pituitary, adrenals, thyroid, ovaries and the testes for men all work in harmony. According to Chris Lamont the main strategy with women going to through Perimenopause transition is to mitigate the lost estrogen production as much as possible using two classes of herbs.
- The Hormone Balancers
- The Phytoestrogens
There are some Herbs which have a natural ability to balance reproductive hormones. And there are different herbs for men and women. Phytoestrogenic plants mimic our own endogenous estrogen. All cells have estrogen receptors on the surface and prior to Perimenopause enough estrogen is produced to be compared as the key that fits into the lock, which is the receptor. When the key is in the lock, then the door opens, and that creates a whole cascade of events that happen inside the cell.
Phytoestrogenic plants are a key that fits into the same lock as the estrogen cell receptor. But it opens the lock partially. We do get a cascade of events happening in the cell similar to when our own homemade estrogen fits there, but it’s a muted reaction. In younger women when they have hormone imbalances it is usually estrogen dominance, having a weaker estrogen in that lock that reduces the overall estrogenic load. But in Perimenopause there is an estrogen deficit, that partial activation of the estrogen receptor can improve the estrogen picture. This will make the Perimenopause transition smoother. That is the reason Phytoestrogens are part of a herbal formula for Perimenopausal woman and is the foundational layer that will reduce symptoms. For some real magic we can add more specific herbs to target the specific symptoms that a particular individual is experiencing.
What if you are low in progesterone?
As a woman moves through Perimenopause, progesterone is also produced in lesser amounts. During a woman’s reproductive years there is an important ratio between estrogen and progesterone. Estrogen dominance may not necessarily be too much estrogen, it might also be not enough progesterone. This is where the hormone balancing herbs play an important role. Herbs like Vitex – ‘chaste tree berry’ act more on progesterone than estrogen. As a preventive measure we can support the liver, which plays an important role in the breakdown and elimination of reproductive hormones and fortifying the adrenal glands. As we know when the ovaries stop producing estrogen, the adrenals take over. If the adrenal glands are overtaxed or fatigued due to chronic stress over the years, then they’re not going to be able to perform well making the midlife transition more bumpy.
In summary, herbs are a lot less aggressive group than the pharmaceutical group. But it may take a little longer than the pharmaceuticals. With a holistic healing modality like herbal medicine, nutrition, and lifestyle the interest is not just in relieving symptoms but also getting to the root cause of health issues. And those root causes are often found in our diet and our lifestyle. The mind body spirit are all interconnected. Herbs compared to drugs are gentler and a lot safer because we can also avoid the nasty side effects of the pharmaceutical medications. The downside is that they work much slower in a lot of cases but they some herbal treatments may respond quickly depending on the symptoms. Hot flashes, night sweats tend to respond really quickly. Mood swings take a little longer. And that is because it’s complicated in terms of balancing hormones, boosting that estrogenic response or it might also be a case of improving gut health, which takes a long time to fix. Chronic conditions and depression take over a month of response time.
If you’re a midlife woman struggling with weight gain? insomnia? mood swings? Get off the hormonal roller coaster ride and download your FREE Perimenopause Rescue Guide here.
To be continued…
In our next session we talk about other symptoms of Perimenopause and discuss some case studies to empower our listeners and women all over the world to discover such wonderful, holistic herbal therapies that help us thrive in the pursuit of good health, happiness, and vitality as we age. Stay tuned!
Check out this amazing Garlic & Herbs Baked Salmon recipe to help you get the nutrients you need during the midlife transition here.

